… continued from Chapter Two of Ethiopia’s Daughters
Chapter Three
A small unlocked Nokia cell phone with an Ethiopian SIM card floats between the white pockets of Dr. Philippa and myself. The number is scribbled on paper taped in the maternity ward. We are on call 24 hours a day, 7 days a week for almost four weeks. Other medical teams before us have stayed for three months, a feat I find holy.
Philippa and myself. The number is scribbled on paper taped in the maternity ward. We are on call 24 hours a day, 7 days a week for almost four weeks. Other medical teams before us have stayed for three months, a feat I find holy.
Nurse midwives and doctor’s names fill our phone lists and tonight it is Abraham* who rings us two hours before midnight. ‘There is a woman in the delivery room, we have tried a vacuum delivery twice and still the baby doesn’t come out, there is fetal distress, can you come and help us?’
‘We are leaving now, right away, be there in 5 minutes.’ I pull on my pants, grab my head lamp and retrieve Dr. Philippa from next door. In our tiredness, we stumble over the dark path, rushing to get to the hospital.
Once inside, the scene is portrayed and everyone rushes to play their part. She is on the stirrup table, her legs shaking from long hours of pushing. One defeated midwife holds the vacuum attached inside the mother, another leans into her protruding belly counting the fetal heart rate, 140 beats per minute down to 80, there is fetal distress, this baby needs to be delivered immediately.
I turn to Dr. Philippa, ‘A C-Section, forceps, what shall we do?’ Calmly, she reassures the team, examines the patient and announces the head is transverse, lying sideways and therefore wedged tight. The goal is to turn the head so delivery can happen. It is too late for a C-Section she informs me.
With fifteen years of experience, she works with her hands, the vacuum, limited tools. An episiotomy opens the narrow passage further and within several minutes a head, with cord wrapped tight about the neck, is pulled through the canal. Deftly, Dr. Philippa reaches for clamps and scissors, releasing the cord. She turns, handing the blue, lifeless baby to Malsaman and me.
‘We should order a Neonatal Resuscitation book and leave it at the hospital,’ Philippa mentioned to me in passing a few months back, I took her recommendation to heart and three days later Amazon delivered such a book. I devoured the algorithms, protocols and ratio of compressions to breaths, the book is for high end facilities with oxygen tanks, neonatal bed warmers and medications. Everything our hospital in Ethiopia is lacking.
Malsaman and I grab the floppy baby, its eyes closed, mouth open, and rest it on the table. An eternity churns before I understand what is before me. ‘I feel a heart beat, its slow, but its here,’ Dr. Philippa presses the umbilical cord, searching for a pulse.
The race begins, from the smallest of compressions, 1 and 2 and , two finger tips thumping the frail chest, the lungs have yet to 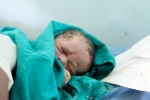 fill with air and the tiny oxygen mask is held in place, I try to keep the airway open, jaw thrust up. It swollen lumpy head lists to the left, making the ability to maintain an airway difficult. For thirty minutes, I don’t give up, I can’t give up.
fill with air and the tiny oxygen mask is held in place, I try to keep the airway open, jaw thrust up. It swollen lumpy head lists to the left, making the ability to maintain an airway difficult. For thirty minutes, I don’t give up, I can’t give up.
A cough, a gasp, the heart beat quickens, we push air into her lungs, ‘come on baby, come on, you can do it,’ my mantra begins. Then it happens, her little chest begins to rise, she takes a breath and then another.
Turning to Malsaman, we are ecstatic and dance around, grasping hands, overcome with joy.
 The mother watches from the delivery table, her feet in stirrups as Philippa delivers the placenta and sews beautifully her torn body back together. Finally, the family is allowed to enter, husband escorts his wife back to bed, there are no wheelchairs. The baby is brought to her side, she is surrounded by four other maternity beds in a small room. Here, there are no monitors, machines or oxygen tanks to keep life viable, only the mother. For she will keep watch, infant at her breast, and hope the spirit of death passes over.
The mother watches from the delivery table, her feet in stirrups as Philippa delivers the placenta and sews beautifully her torn body back together. Finally, the family is allowed to enter, husband escorts his wife back to bed, there are no wheelchairs. The baby is brought to her side, she is surrounded by four other maternity beds in a small room. Here, there are no monitors, machines or oxygen tanks to keep life viable, only the mother. For she will keep watch, infant at her breast, and hope the spirit of death passes over.
 Not much later, the cell phone rings, another midwife urgently inviting us back. ‘Another baby is stuck, she has been in labor since yesterday, we should go quick,’ Philippa informs me, grabbing her white coat and we walk the well trotted path together. The story parallels the first, only the cord is wrapped around three times, strangling any chance of survival. This time our attempts are futile, the little face is malformed, perhaps a chromosomal defect, an incomplete cleft palate, perhaps it is from pushing, its face lodged against the canal bones for too long.
Not much later, the cell phone rings, another midwife urgently inviting us back. ‘Another baby is stuck, she has been in labor since yesterday, we should go quick,’ Philippa informs me, grabbing her white coat and we walk the well trotted path together. The story parallels the first, only the cord is wrapped around three times, strangling any chance of survival. This time our attempts are futile, the little face is malformed, perhaps a chromosomal defect, an incomplete cleft palate, perhaps it is from pushing, its face lodged against the canal bones for too long.
I can’t fix the oxygen mask, air escapes before passing into underdeveloped lungs. The ailing heart pulses through the cut cord, ‘thump …….. thump.……..’ instead of a healthy 120 beats/min, there is only one every five seconds. More compressions, more oxygen, the heart beat slips further into the heavens, we try and try again. ‘Come on baby, come on, you can do it,’ my mantra begins, only this time no one is listening and over 30 minutes the little soul leaves us.
Looking into Malsaman’s eyes, a wave of defeat overcomes the room. I want to cry, but no one cries in Africa, there is too much sorrow for tears.
‘We have saved the mother,’ he touches my shoulder, now they can have more children, healthy children.’
* names have been changed
to be continued…



 Follow
Follow
February 17th, 2011 by becca
Those little beings are lucky to be in the presence of your love, determination, and strength….
February 9th, 2011 by bill and donna
once again i feel the pain you endure everyday.i’m just so proud of the work you and jay are doing along with everyone else there. you and jay will be awarded by your friendships that will follow, the lives you have given hope to. dad
February 7th, 2011 by Karly aka Sista
Your amazing Darlene
February 7th, 2011 by Karly aka Sista
Yuri and I watched A Walk to Beautiful… Really good documentary and good way to learn more about what your doing.
Miss you and love You
February 6th, 2011 by Dianne / Mom
Darlene, that was exhilerating and heartbreaking.
February 5th, 2011 by Janelle
What a night, I will cry those tears for you. Victory and Sorrow!!!
February 5th, 2011 by Annie Valentine
Your stories and pictures touch me as few others. You are superheroes on my book.